Alaska Blind Child Discovery
A
cooperative, charitable research project to vision screen every preschool
Alaskan
preK and 3rd in Alaska Schools
Home
Reduction of Amblyopia by Enhanced Detection in Schools: READS
Background:
The purposes of early school vision screening are 1) to detect amblyopia while it is treatable, and also 2) to render children’s vision clear enough to allow learning. Typical American School vision screening relies on 1) charts with various optotypes, 2) various distances such as 20 feet, 3) various methods to cover the untested eye. Despite adherence to such guidelines, school screening is not working as well as possible; some children with amblyopia fail to be detected (insufficient sensitivity) and many normal children are sent for confirmatory exams that they really don’t need(insufficient specificity). A recent such case of acuity screen referral from Adak resulted in $3000 cost to public insurance only to find the student didn’t even need glasses. Amblyopia is a deficient brain learning of vision due to disrupted or double vision in the critical first decade of life(Simons 2005; Wu and Hunter 2006).
School nurses would prefer a test with equal or better validity that is inexpensive, efficient and quick.
The public should demand results for their tax dollars. Unlike the high-school exit exam that attempts to quantify learning for all students in a region, there is NO uniform measure of community-based success regarding amblyopia detection and therapy.
In the spring of 2004, enhanced flip card acuity testing was compared to two objective photoscreening techniques in about one third of Anchorage Elementary Schools. 1700 students, First grade, kindergarten and pre-K were screened. 243 Had confirmatory exams and another 1300 had completely normal acuity and photoscreening. From these, the sensitivity and specificity for the screening tests was estimated against a pre-defined Gold-Standard(Donahue et al. 2003).
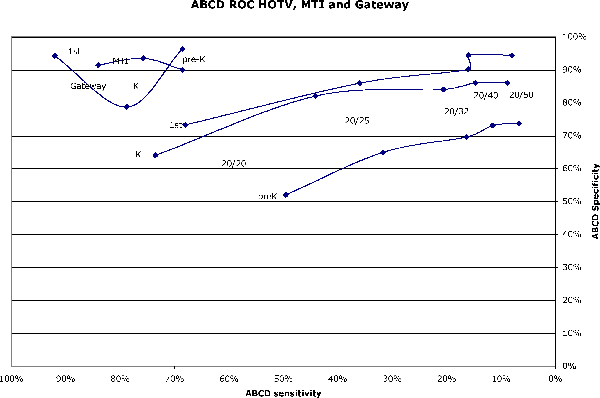
Sensitivity (ability to detect children with disease) plotted against specificity (normal children do not need confirmatory exam) for patched flip-card HOTV acuity testing at given thresholds and two photoscreeners (MTI and Gateway). The more valid tests are in the “northwest corner” of the graph(Leman et al. 2005a).
Acuity testing was made more specific by immediately retesting each student unable to pass the initial threshold level, first with a pinhole over the un-patched eye, and second with a near acuity card. The photoscreening, first with a portable digital Gateway DV-S20 camera(Arnold et al. 2004) and then with the time-tested MTI Polaroid photoscreener(Ottar et al. 1995; Donahue et al. 2000; Arnold et al. 2000), was done in portable tents that afforded a non-distracting, luminance-shielded area near the classroom{Arnold, 2006 #1625}. Photoscreens were physician interpreted using the delta-center crescent method(Kovtoun and Arnold 2004). Acuity testing took about 150 seconds while photoscreening took only about 30-40 seconds. The positive predictive value (proprtion of referred students with real disease) was 80% for patched acuity testing and 80-90% for photoscreening(Leman et al. 2005b). This data was presented and well-received at the National School Nurses Meeting in Washington DC July 2005.
Preschool vision screening combined with active amblyopia therapy results in a substantial reduction in the prevalence of residual amblyopia vision impairment(Eibschitz-Tsimhoni et al. 2000; Kvarnstrom et al. 1998; Williams et al. 2003). Vision screening has high societal cost-effectiveness{White, 2004 #1491;Arnold, 2006 #85} and meets the muster of evidence-based medicine(Calonge and USPSTF 2004).
The National Institutes of Health has recently supported a multicenter preschool study to determine the most sensitive methods for vision screening preschoolers. In this collaborative effort between academic optometrists and ophthalmologists called the Vision in Preschoolers Study (VIPS), patched acuity testing with LEA symbols and remote autorefraction with the Welch Allyn sight initially appeared to outdo photoscreeners when performed by doctors(VIPS 2004), however these tests were not as good when performed by nurses and lay-screeners(VIPS et al. 2005). The predictive value of Welch Ally Suresight is quite low (30-40%) despite enhanced referral criteria different from manufacturer as generated via VIPS(Hudson and Donahue 2005).
Proposed Study
Kindergarten:
All Kindergarten students with appropriate consent will be formally vision screened. Each will have acuity tested with an adhesive patch over the non-tested eye while attempting to read or match surround HOTV letters on a flip-card from a pre-defined distance of 10 feet. Then a digital photoscreen will be taken of each student in the same 6 long ft x 4 ft high by 2.5 feet wide darkened tent. The photoscreens will be physician interpreted with results sent back to each school nurse, and mailed to each parent. Each student who fails either the photoscreening and/or the acuity testing will be notified that they should receive a confirmatory eye exam from their nearest convenient eye doctor, unless they provide evidence of a recent eye exam. If the school nurse identifies any such referred students as unable to afford an eye exam, then a no-charge exam will be provided by the ABCD Coordinating Center.
Third Grade
All Third Grade Students with appropriate consent will be formally screened. All those capable of using a computer will have acuity and depth perception tested on the “Amblyopia Foundation of America” Computer Game screening test at a distance of 8 feet. Those failing this computer screen will take a routine patched 10-foot surround HOTV acuity test for confirmation. The school nurse may have medical information on the etiology of decreased acuity for many of these students. On the other hand, newly detected acuity decrease students will be referred for a confirmatory exam from their nearest convenient eye doctor. School nurses may refer financially needy students for no-charge exams from the ABCD Coordinating Center.
Data Collection
The ABCD Coordinating Center will confidentially collect results from the Consent Forms, The acuity Tests and the photoscreen interpretations and then attempt to retrieve as many confirmatory exams as possible. School nurses will receive follow up from confirmatory exams on referred patients. For third graders, as attempt will be made to quantify the prevalence of residual amblyopia (acuity not better than 20/32) in the school district. A receiver-operator characteristic curve will be generated on “silver-standard” confirmatory exam outcomes for acuity thresholds in Kindergarten and for the “Amblyopia Foundation of America” Vision Quest computer Game acuity in third graders. The Vision Quest results will be directly compared to patched HOTV acuity for the first three schools (200 students) as a baseline.
Cost
The ABCD Coordinating Center will assume the cost of:
The Research Student Coordinator (Michelle Clausen, BA)
The Photoscreeners and Interpretation
The Photoscreen Tents
The Consent paperwork
The Acuity Test Cards
The Patches for acuity testing
The Vision Quest Software and Red-Blue Spectacles
Up to 2 computers for Vision Quest with 8-foot mouse extensions
Mailing results to parents
Collecting Data and reporting back to school district
Reward for school nurse recruiting the highest percent of students for consent
School nurse referral for confirmatory exams due to financial need
Summary
The Spring 2004 ASD-ABCD study brought an enhanced, portable acuity test that was completed by a higher percent of younger elementary students than with existing methods. ASD-ABCD documented speed advantages of objective testing and that photoscreening outperformed acuity testing with respect to estimated sensitivity and specificity for target amblyogenic conditions. Digital photoscreening (with physician interpretation) was equally inexpensive per student as flip-card patched acuity testing, but would have been less expensive if nurse time had been included{Leman, 2005 #1454;Leman, 2005 #1633;Arnold, 2006 #1625}.
The Spring 2006 Study will offer this improved to all Kindergarten students in the district. Third graders will be sensitively screened for residual amblyopia at an old enough age that formerly treated amblyopia gains should be retain good vision, but at an age when implementation of intense amblyopia therapy still may have substantial gains in a newly-diagnosed student(Mohan et al. 2004; PEDIG et al. 2005).
This will be a prototype of an efficient method for determining regional rates of residual amblyopia; a cost-effective variable never before collected in America.
Presented by:
Robert W. Arnold, M.D.
Reduction of Amblyopia by Enhanced Detection in Schools: RAEDS
References:
1. Simons K. Amblyopia characterization, treatment and prophylaxis. Surv Ophthalmol 50: 123-166, 2005.
2. Wu C and Hunter DG. Amblyopia: Diagnostic and Therapeutic Options. Am J Ophthalmol 141: 175-184 e172, 2006.
3. Donahue S, Arnold R and Ruben JB. Preschool vision screening: What should we be detecting and how should we report it? Uniform guidelines for reporting results from studies of preschool vision screening. J AAPOS 7: 314-316, 2003.
4. Leman RE, Armitage MD and Arnold RW. The receiver-operator curve for flip-card surround HOTV in younger school children. Am Orthopt J 55: 128-135, 2005a.
5. Arnold RW, Arnold AW, Stark L, Arnold KK, Leman RE and Armitage MD. Amblyopia detection by camera (ADBC): Gateway to portable, inexpensive, vision screening. Alaska Med 46: 63-72, 2004.
6. Ottar WL, Scott WE and Holgado SI. Photoscreening for amblyogenic factors. J Pediatr Ophthalmol Strabismus 32: 289-295, 1995.
7. Donahue SP, Johnson TM and Leonard-Martin TC. Screening for amblyogenic factors using a volunteer lay network and the MTI photoscreener. Initial results from 15,000 preschool children in a statewide effort. Ophthalmology 107: 1637-1644; discussion 1645-1636., 2000.
8. Arnold RW, Gionet E, Jastrzebski A, Kovtoun T, Armitage M and Coon L. The Alaska Blind Child Discovery project: Rationale, Methods and Results of 4000 screenings. Alaska Med 42: 58-72, 2000.
9. Arnold RW, Stark L, Leman RE, Arnold KK, Bates J and Armitage MD. Tent photoscreening and patched acuity by school nurses: Validation of ASD-ABCD. J AAPOS In press, 2005a.
10. Kovtoun TA and Arnold RW. Calibration of photoscreeners for threshold contact- induced hyperopic anisometropia: Introduction of the JVC photoscreeners. JPOS 41: 150-158, 2004.
11. Leman RE, Arnold RW, Arnold KK, Stark L, Armitage MD and Bates J. Implementation of patched acuity testing and photoscreening by school nurses. J School Nursing 21: submitted, 2005b.
12. Eibschitz-Tsimhoni M, Friedman T, Naor J, Eibschitz N and Friedman Z. Early screening for amblyogenic risk factors lowers the prevalence and severity of amblyopia. J AAPOS 4: 194-199, 2000.
13. Kvarnstrom G, Jakobsson P and Lennerstrand G. Screening for visual and ocular disorders in children, evaluation of the system in Sweden. Acta Paediatr 87: 1173-1179, 1998.
14. Williams C, Northstone K, Harrad R, Sparrow JM, Harvey I and ALSPAC-Study-Team. Amblyopia treatment outcomes after preschool screening v school entry screening: observational data from a prospective cohort study. Br J Ophthalmol 87: 988-993, 2003.
15. White A. Costs and Benefits of Comprehensive Eye Exams: Abt Associates, 2004.
16. Arnold RW, Armitage MD, Gionet EG, Balinger A, Kovtoun TA, Machida CJ and Coon LJ. The cost and yield of photoscreening: Impact of photoscreening on overall pediatric ophthalmic costs. JPOS 42: 103-111, 2005b.
17. Calonge N and USPSTF. Screening for visual impairment in children younger than 5 years: Recommendation Statement. Ann Fam Med 2: 263-266, 2004.
18. VIPS. Comparison of preschool vision screening tests as administered by licensed eye care professionals in the vision in preschoolers study. Ophthalmology 111: 637-650, 2004.
19. VIPS, Dobson V, Quinn G, Kulp MT, Cyert L, Ciner EB, Ying G-S, Moore B, Redford M, Orel-Bixler D, Baumritter A and Schmidt P. Preschool vision screening tests administered by nurse screeners compared with lay screeners in the Vision in Preschoolers Study. IOVS 46: 2639-2648, 2005.
20. Hudson A and Donahue S. Review of results of pre-school vision screening. Invest Ophthalmol Vis Sci 46: Eabstract 686, 2005.
21. Mohan K, Saroha V and Sharma A. Successful occlusion therapy for amblyopia in 11- to 15-year-old children. JPOS 41: 89-95, 2004.
22. PEDIG, Scheiman MM, Hertle RW, Beck RW, Edwards AR, Birch E, Cotter SA, Crouch ER, Jr., Cruz OA, Davitt BV, Donahue S, Holmes JM, Lyon DW, Repka MX, Sala NA, Silbert DI, Suh DW and Tamkins SM. Randomized trial of treatment of amblyopia in children aged 7 to 17 years. Arch Ophthalmol 123: 437-447, 2005.
ABCD History
Kids Eye Disorders
Amblyopia
Vision Screening
Issues
ABCD Clinics
References
Contact ABCD